Inspira is among the first 100 hospitals nationwide to adopt the new Monarch™ navigational...
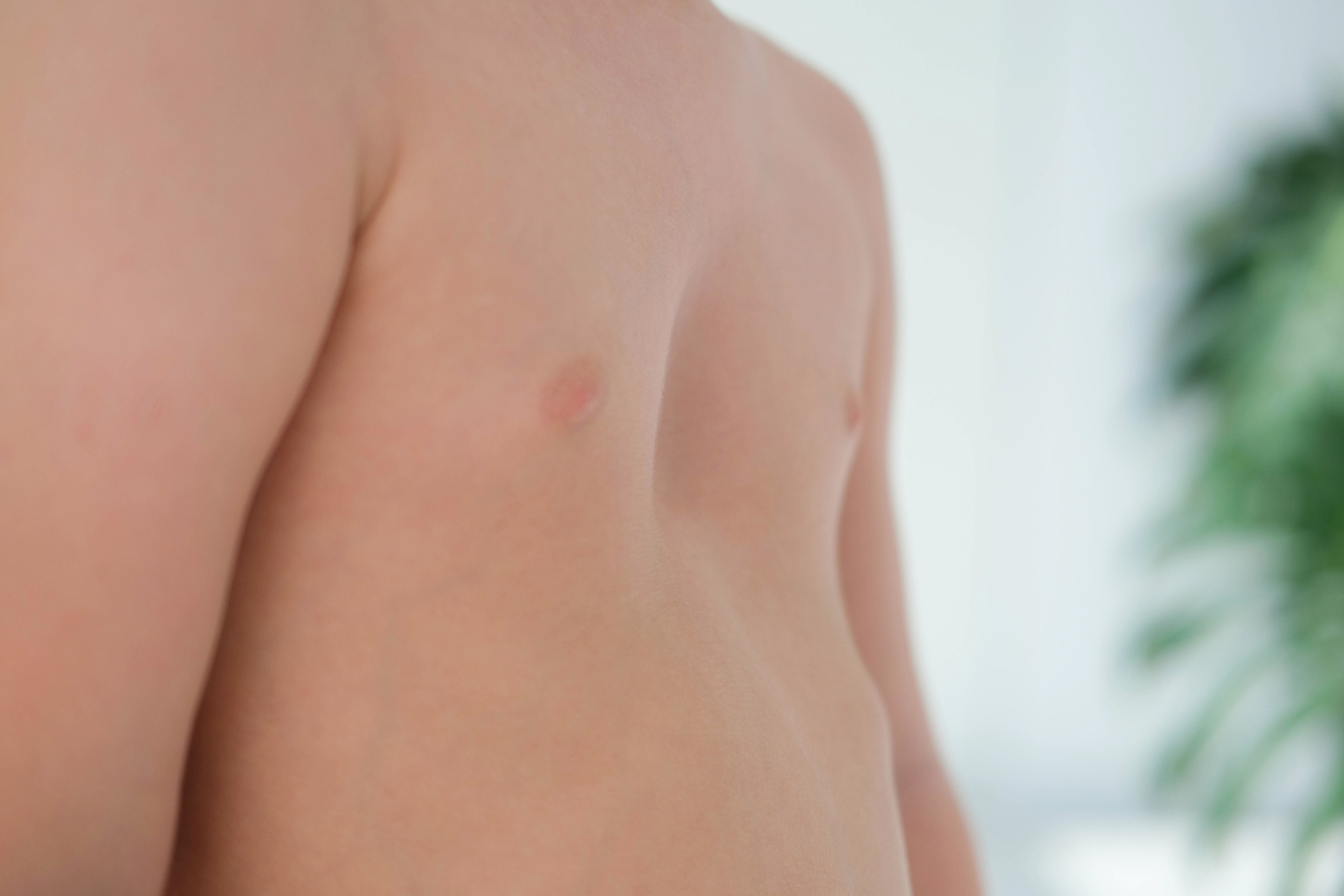
A sunken or indented chest can be more than a cosmetic concern. Sunken chest, also known as pectus excavatum, occurs when the breastbone (sternum) curves inward, creating a noticeable dip in the chest.
While some people experience mild symptoms, others may develop breathing issues, chest discomfort or a reduced exercise tolerance.
“Pectus excavatum, the most common type of chest wall deformity, often becomes more noticeable during childhood or adolescence, especially during growth spurts,” said Christopher C. Derivaux, MD, thoracic surgeon at Inspira Health. “The condition can affect the position of the heart and lungs, potentially limiting their function, especially during physical activity.”
Pectus excavatum symptoms vary widely. Some individuals have no physical complaints but may feel self-conscious about the appearance of their chest. Others may experience shortness of breath, fatigue, chest pain or frequent respiratory infections. Thoracic specialists use imaging, lung function tests and heart assessments to evaluate the condition’s severity and determine whether treatment is appropriate.
Not everyone with pectus excavatum needs surgery. Treatment decisions are based on a combination of physical symptoms, imaging findings and the condition’s impact on overall quality of life. Surgery is more commonly recommended when the chest indentation interferes with heart or lung function or causes significant discomfort or exercise intolerance.
For some adolescents and adults, body image concerns related to pectus excavatum can affect confidence, social participation and emotional well-being, which may factor into treatment discussions.
There are two primary surgical approaches for correcting pectus excavatum, which both reposition the chest wall and improve function:
A thoracic surgeon will recommend the most appropriate option based on your age, anatomy, condition severity and overall health.
Surgery can provide both physical and emotional benefits for patients who are strong candidates. Many people experience improved breathing capacity, increased stamina and reduced chest discomfort following recovery. Correcting the chest wall position can also improve heart function in cases of compression.
Many patients report improved self-confidence and comfort with their appearance after surgery, which can positively affect daily life and mental well-being.
“Recovery varies from patient to patient depending on the surgical approach, but most people spend several days in the hospital for pain control and monitoring,” said Dr. Derivaux. “Pain management is an important part of recovery, especially in the early weeks, and activity restrictions are common while the chest heals.”
Your doctor may advise you to avoid heavy lifting and contact sports for a period of time while gradually returning to normal activities. Follow-up appointments help ensure proper healing and monitor progress. For those who undergo the Nuss procedure, a second surgery is planned years later to remove the support bars once the chest has stabilized.
If you or your child has pectus excavatum and experiences symptoms or concerns, a thoracic specialist can help you determine the appropriate next steps. Evaluation and treatment are highly individualized, and advances in surgical techniques continue to improve outcomes and experiences.
Early consultation helps patients and families understand their options and make informed decisions about their care. With the right approach, many individuals with pectus excavatum can achieve better function, comfort and confidence.
Schedule an appointment with a thoracic specialist at Inspira.

Inspira is among the first 100 hospitals nationwide to adopt the new Monarch™ navigational...
To help better understand what treatment options are available to patients, Charles Shieh, M.D...